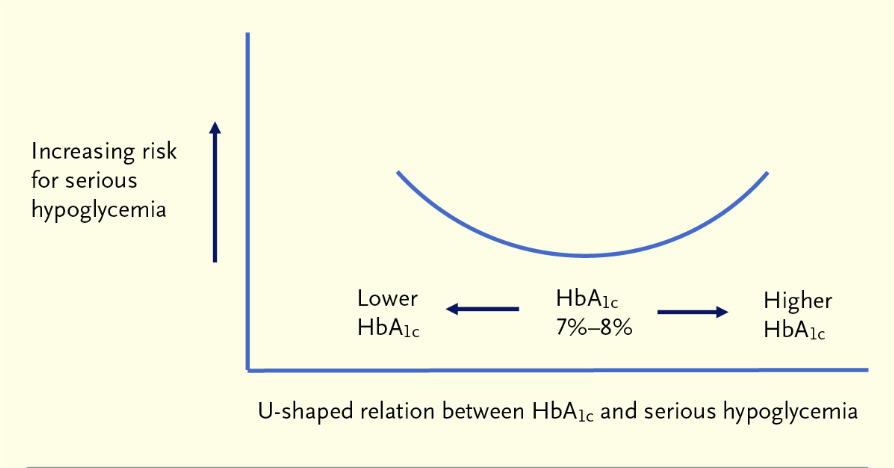
Serious Hypoglycemia at Both High and Low Glycosylated Hemoglobin Levels
In a study published in 2013, serious hypoglycemia was associated with both high (>9%) and low (<6%) levels of glycosylated hemoglobin (HbA1c) in patients with type 2 diabetes — a so-called U-shaped association (NEJM JW Gen Med Jan 15 2014 and Diabetes Care 2013; 36:3535). Now, another research group has examined this issue.
U.K. researchers identified 304 patients with type 2 diabetes who had a first hospitalization for severe hypoglycemia and underwent HbA1c testing within the previous 90 days. These cases were compared with 304 controls — matched by age, sex, duration of diabetes, and other relevant clinical characteristics — who were not hospitalized for hypoglycemia. Compared with HbA1c of 7.0%, HbA1c levels of 6% and 9% conferred excess risk for hypoglycemia-related hospitalization (odds ratios, 1.5 for both). For HbA1c between 4.0% and 6.5%, the lower the HbA1c level, the higher the risk for hypoglycemia. For HbA1cbetween 8.0% and 11.5%, the higher the HbA1c level, the higher the risk for hypoglycemia (see figure).
COMMENT
This study, like its 2013 predecessor, showed a U-shaped association between HbA1c level and hypoglycemia. The correlation between low HbA1c and hypoglycemia clearly represents too-tight glycemic control. The correlation between high HbA1c and hypoglycemia likely is multifactorial, representing combinations of intrinsic glycemic lability and fluctuations in diet, exercise, and adherence to antidiabetic therapy. A take-home message is that clinicians should query all diabetic patients about hypoglycemia consistently, regardless of their HbA1c levels.